 Because there is no known “cure” for TMD, management of patients with TMD symptoms is similar to management of patients with other orthopedic or rheumatologic disorders. The goals of TMD management include decrease in pain, decrease in adverse pressure or “loading” on the jaw joints, restoration of function of the jaw and normal daily activities. These goals are best achieved by identifying all contributing factors and implementing a well-defined management program.
Because there is no known “cure” for TMD, management of patients with TMD symptoms is similar to management of patients with other orthopedic or rheumatologic disorders. The goals of TMD management include decrease in pain, decrease in adverse pressure or “loading” on the jaw joints, restoration of function of the jaw and normal daily activities. These goals are best achieved by identifying all contributing factors and implementing a well-defined management program.
The pain and discomfort associated with most TMJ disorders can be managed with conservative, self-managed care or non-surgical therapies. Therapy for TMJ problems can range from simple measures to extensive therapy. This may include physical therapy, exercises, nutritional recommendations and the use of stress reduction techniques, medications and trigger point injections.
Physical therapy modalities are often required to return the muscles to normal comfort and function. These might include moist heat, ultra-sound, massage, stretches, transcutaneous electro-neural stimulation (TENS) or electro-galvanic stimulation (EGS).
Such conservative management techniques have proven to be safe and effective in the vast majority of TMD cases. While rarely needed, surgery is sometimes performed when conservative treatment has failed to improve comfort and function. However, even when TMD symptoms are long standing and severe, most patients rarely require invasive treatments designed to permanently change the bite or repositioning of the jaw.
 There is no reason to live with the pain. The risks of leaving TMD untreated simply aren't worth it.
There is no reason to live with the pain. The risks of leaving TMD untreated simply aren't worth it.
Self-Care
For very mild cases, or prior to being able to see a TMD specialist, there are self-management actions you can do for yourself, such as:
-
Limit your jaw opening movement to about two finger widths
-
Avoid chewing hard or very chewy food, or gum
-
Cut food into smaller pieces
-
Massage painful facial muscles
-
Use cold packs or moist heat packs
-
Avoid grinding & clenching your teeth
-
Practice keeping teeth apart and lips together
-
Avoid chewing non-food items, ie: pencils, fingernails, etc.
-
Avoid playing musical instruments that put pressure on your jaw
-
Learn stress management and relaxation techniques
-
Keep a diary of your pain, and anything, or any time of the day or night, that makes it better or worse
Orthodontics
Orthodontics is the field of dentistry treating problems with a person’s bite and alignment of teeth. This is most frequently accomplished with what is known as “braces”. For many years there have been theories that having braces may treat temporomandibular disorders (TMD) when present and others thought braces to cause TMD problems.
Though it is important for one’s health to have a good bite and a stable dentition with which to chew, swallow and speak properly, orthodontics is not commonly a treatment for TMD conditions. The philosophy of treating TMD problems with braces developed decades ago following some faulty research concluding that “occlusal discrepancies”, problems with how the teeth come together (the bite), caused TMD conditions. Many research projects since this time have shown occlusion not to be a primary factor in the development of TMD diseases. Therefore; braces do not treat TMD problems.
Contrarily, there have been groups claiming that orthodontic treatment causes TMD problems. This came about partly because of the temporal relationship of braces and onset of TMD. Most individuals get braces in adolescence and the first age group that tends to develop TMD are the adolescents. But, now there is research spanning more than 30 years showing that populations that had braces and populations without braces have the same incidence of TMD problems. With that said, orthodontic care does create stresses on the teeth, bone and temporomandibular joints (TMJ). These loads on the system may exacerbate, or seem to cause a TMD problem.
An orthodontist will typically assess the TMJs, jaw and facial muscles, opening and closing of the jaw, prior to orthodontic care. Should any problems or concerns be identified the patient will likely be referred for a TMD/TMJ examination with a TMJ specialist. It is vitally important to have all TMD problems stabilized prior to braces. Providing braces to an individual with an unstable TMJ, degenerative joints, inflamed joints, joints with displaced discs or inflamed muscles may result in orthodontic treatment that is unable to achieve and maintain the desired result for the occlusion and teeth positions.
If in orthodontic care now or are contemplating orthodontic care discuss any jaw pain, facial pain, TMJ clicking/popping/grinding, ear pain or headaches with your orthodontist. Or, you may make an evaluation appointment with a doctor that specializes in TMD care at the TMJ & Orofacial Pain Treatment Centers of Wisconsin.
Surgery
Surgery, with respect to TMJ disorders, has changed significantly over the past 50 years. In the past the number of TMJ patients being referred for a surgical procedure was in the range of 15-50%. Many of the surgical procedures once advocated for have now been abandoned due to low success rates and long-term negative consequences. Valuable lessons were learned and many positive changes were made to the surgical indications and protocols. Today, the numbers of patients requiring surgery are minimal, with estimates in the range of 2.5%. At the TMJ & Orofacial Pain Treatment Centers of Wisconsin the percent of those referred for surgical consult is even lower, below 1%.
Often people have a misconception about surgery for TMJ disorders. Unrelenting pain, in itself, is not an indication for surgery, nor is surgery a “quick fix” for TMJ disorders. For surgery to be successful there must be a physical problem that can be corrected by the surgeon. Muscle, nerve, and vascular disorders are not typically amenable to surgical correction. There are some definite indications for surgery such as fractures, infections and neoplasms, but as previously stated the indications are few.
Procedures that may be indicated in those rare circumstances when conservative therapy is less than adequate:
-
Arthrocentesis – flushing of the TMJ to relieve inflammation and remove adhesions that may be preventing a disc from functioning properly.
-
Arthroscopy – flushing of the TMJ, with the added benefit of having a camera port into the joint for the surgeons to visualize and remove adhesions.
-
Arthrotomy – open joint procedures to remove discs, reshape degenerated bone, remove neoplasms, and replace joints with artificial components.
Medication
Medications may be considered in the management of patients with orofacial pain, including TMD. The choices often reflect the acute or chronic pain levels in each individual patient and the presenting signs and symptoms following a diagnosis. Medications may be helpful in improving patient comfort and in rehabilitation when used as part of a comprehensive program. Unfortunately, there is no single drug that has been proven effective for the spectrum of TMD. Therefore medications of various types may be considered in creating the treatment plan of patients with these conditions. Not every patient requires the addition of medication in his or her management, as every treatment plan strives for the most conservative approach possible.
The most widely used types of medications in the management of TMD are analgesics, nonsteroidal anti-inflammatory drugs (NSAIDs), corticosteroids, benzodiazepines, muscle relaxants, and low-dose antidepressants. These medications may be used alone, or in combination for various lengths of time. Every effort is made to avoid long-term use and the lowest dosage is always used to minimize side effect concerns. Occasionally injections are utilized, and the main agents used are local anesthetics and corticosteroids. Lastly, topical medications may be considered and include single agent or a combinations of previous mentioned agents. The other modalities used in a comprehensive program should allow effective treatment for these conditions with a minimal use of medication.
Trigger Points
TRIGGER POINTS (TP) DEFINED: A common reaction to an untreated joint problem anywhere in the body, namely the temporomandibular joint in this instance, is what is referred to as “muscle guarding” which is the body's natural response is to protect or guard itself from further injury. This reflex muscle guarding is in the form of muscle tightening which serves to “splint” the area.
One of the consequences of continued muscle guarding is the development of what is referred to as muscle Trigger Point (TP). TPs can and will develop in any voluntarily controlled muscle, including the jaws, neck, and shoulder muscles, that is continually tight from guarding.
A TP by definition, is a palpable nodules in taut bands of muscle fibers that can develop in any muscle that is continually fatigued from guarding. TPs are felt as painful “lumps” or hard “knots” which can be felt fairly easily when a muscle is palpated or felt and when a TP is pushed or prodded with the fingers during a physical examination.
In a TMD patient, TPs will develop not only in the chewing muscles but also in the associated neck and shoulder muscles leading to commons symptoms often reported by TMJ disorder patients such as: 1) limited opening of the jaws, 2) pain when eating, 3) bite feels off, 4) headache to name a few.
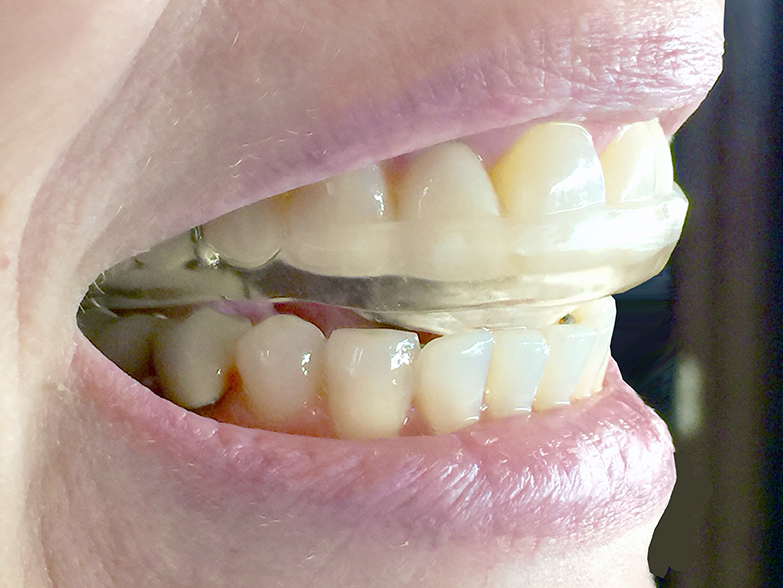
TREATMENT: Effective treatment of TP pain first requires stabilizing the jaw joint which is causing the muscles to remain guarded which is accomplished by the use of an intraoral device often called a “splint” which when in place, will reduce pressure within the TM joints thereby reducing the need to for the muscles to remain guarded. Once this is accomplished, direct treatment to the TPs will be much more effective. Some common treatment approaches of the muscles with TPs, is accomplished with physical therapy (PT), dry-needling/TP injection, postural improvement & re-education to name some of the more common methods. Equally important is the patient’s participation from daily, self-directed care of the muscles (self-massage & stretching) and improving muscle tone through exercise.
Diagnostic Nerve Block
BACKGROUND: the process of sorting through the maze of reasonable possibilities of what condition and/or from where is the source of pain is often referred to as "working the Differential Diagnosis".
Definition of Differential Diagnosis: “the distinguishing of a disease or condition from others presenting with similar signs and symptoms”. Confirming the diagnosis before beginning definitive treatment is often times advisable, especially if the patient has had the pain for a long time and has previously undergone therapy and failed to respond. There a several accepted methods that can assist the clinician in confirming the proposed diagnosis or to narrow the differential diagnosis.
One of the more common and effective methods to localize the source of pain is the anesthetic blocking of of related tissues referred to here as Diagnostic Analgesic Blocking or “DAB”.
Instruments/supplies used for a DAB: This procedure utilizes instruments common to any dental or medical practice, namely: a syringe with a 25 or 27-gauge needle, topical anesthetic or “numbing gel” if the injection will be within the mouth or, ice/cold spray (aka: Vapocoolant spray) for topical numbing of the skin, both applied before the injection, and injectable anesthetic such as 1% lidocaine or 0.5% bupivacaine, alcohol or iodine wipes to cleanse the skin for extraoral injections and cotton gauze sponges for control of any bleeding after an injection which is often very minimal.
Using DAB to arrive at a diagnosis: Next, a review of the patient’s chief complaints; a pain diagram (seen to the right) is very helpful. in this example case, the patient complains of pain in the following areas: 1) headache in the left temple region, 2) left earache, 3) left pain at the angle of the jaw and 4) left teeth pain. Pain experienced in these areas may be referred pain from: an infected ear, infected or split molars, cluster migraine, left side temporomandibular joint inflammation. Let us assume that this patient has been seen by a neurologist for migraine cluster headaches, by an ENT specialist for ear infection, and a dentist for dental problems and all have reported negative findings, what next? What else could explain these pain problems?
What to the pain charts tell us: From the pain chart of the trapezius muscle and masseter muscle, we can see that 1) the trapezius muscle can refer pain to the temple and b) that jaw the masseter muscles can refer pain to the upper & teeth.
Now what is done? We can sequentially anesthetize a) left upper trapezius which may eliminate the temple but not the teeth pain, so next, we may anesthetize b) masseter muscles. If teeth pain is then temporarily eliminated, this DAB procedure has rendered a positive (+) diagnostic response, and we are one more step closer to controlling or curing this pain problem.
Crown/Bridge
In the past a theory had developed that occlusion (the way the bite comes together) caused temporomandibular disorders (TMD). This was the result of a poorly designed research project perpetuating this idea. There are practitioners today that still hold to the theory that treating what they believe to be problems with a person’s occlusion (bite) is the appropriate care for TMD issues. Though the occlusion may contribute, it is not common for the occlusion to be the primary source for a TMD problem.
Crowns (“caps”) and bridges are artificial devices fabricated to replace and restore fractured teeth, teeth damaged by cavities, and missing teeth and are vitally important in maintaining a stable occlusion. This may be part of an overall care plan for the management of TMD, but is certainly not the norm for TMD care. We, at the TMJ & Orofacial Pain Treatment Centers of Wisconsin, do not provide crown and bridge care, your family dentist is the expert for this type of dental care. Our center follows the protocols for conservative care of orofacial pain disorders in accordance with the guidelines of the National Institute of Health (NIH) and the American Academy of Orofacial Pain (AAOP).